부모 교육이 보완대체의사소통 인식에 미치는 영향
The Effects of Parent Education on Perceptions of Augmentative and Alternative Communication
Article information
Abstract
배경 및 목적
AAC에 대한 부모의 부족한 지식은 오해와 편견을 야기할 수 있으며 이는 자녀에게 적절한 중재를 제공하는 데 있어 방해 요인으로 작용할 수 있다. 이에 본 연구는 부모 교육이 AAC에 대한 인식 변화에 영향을 미치는지를 살펴보고자 하였다.
방법
복합적인 의사소통 요구를 지닌 아동을 둔 25명의 어머니가 본 연구에 참여하였다. 부모 교육은 (1) 보완대체의사소통 이해하기, (2) 다양한 AAC 도구 살펴보기, (3) AAC로 의사소통능력 향상하기, (4) 가정에서 쉽게 AAC를 활용하는 팁, (5) AAC 지원정책 알아보기로 구성된 40분의 프로그램으로 설계하였으며 여기에 질의응답 시간을 추가하였다. 부모 교육이 AAC 인식에 미치는 영향을 살펴보기 위해, 그리고 부모의 인식 변화 정도와 교육 프로그램에 대한 만족도 간의 상관관계가 있는지를 살펴보기 위해 AAC 인식 관련 설문지와 교육 프로그램 만족도 설문지를 개발하였다.
결과
t-test와 ANCOVA 분석 결과 AAC 인식에 관한 모든 설문 항목의 평균 점수가 교육 후 증가하였고 교육 전후의 점수 차이는 모두 유의한 것으로 나타났다. Spearman 상관계수는 .443으로 만족도 점수와 AAC 인식 변화 간에 중간 정도의 양적 상관관계가 있는 것으로 나타났다.
논의 및 결론
본 연구는 부모교육이 AAC에 대한 부모의 인식에 긍정적인 영향을 미친다는 것을 보여주었다. 특히 아동이 AAC를 사용하기 위해서는 온전한 인지능력을 갖춰야 한다는 잘못된 인식에 대해 가장 큰 변화가 관찰되었다. AAC에 대한 인식 개선과 관련 정보 및 기기 사용 기회의 제공에 중점을 둔 부모교육 프로그램이 긍정적인 인식 변화를 이끌어 낸 것으로 보인다.
Trans Abstract
Objectives
Parents’ incomplete knowledge of AAC is apt to make them believe in misconceptions about AAC, which hinders them from having the appropriate interventions for their children. Considering the fact that parents’ perception of AAC has a large impact on AAC intervention, this study aims to examine the effects of parent education on the perception of AAC.
Methods
Twenty-five mothers of children with complex communication needs participated in the study. Parent Education is designed as a 40-minute program consisting of (1) introduction to AAC, (2) exploring AAC systems, (3) developing linguistic competence using AAC, (4) tips for using AAC at home, and (5) policies and financial support. Extra time for question-and-answers was provided to each participant. To measure the effect of parent education on parents’ AAC perception and the relationship of participants’ change in perception with their satisfaction with the education program, two types of survey questionnaires were developed.
Results
The repeated measured ANCOVA showed that the difference between the total scores of pre-and post-surveys was significant. The Spearman’s rho was .443, indicating a moderate positive correlation between the degree of satisfaction and the change in AAC perception.
Conclusion
This study showed that parent education had a positive effect on parents’ perceptions of AAC overall. In particular, there was a significant change of opinion in the misconception that children must have intact cognitive skills to use speech-generating devices, the idea which showed the lowest scores in the pre-survey. It seems that the education program which focused on correcting misconceptions about AAC and providing relevant information and opportunities to use AAC devices helped to lead to these positive effects.
Parents’ participation in augmentative and alternative communication (AAC) has been emphasized (Huer & Lloyd, 1990). Parents of children with complex communication needs (CCN) play an important role as informants in AAC evaluation and interventional goal setting, in addition to taking responsibility for implementing AAC in practice in their daily life (Granlund, BjÖrckÅKesson, Wilder, & Ylvén, 2008; Marshall & Goldbart, 2008; Park, 2020, 2021). Their involvement in the overall AAC decision-making process can lead to successful use of AAC by their children (Kent-Walsh, Binger, & Hasham, 2010; Seligman-Wine, 2007; Thunberg, Sandberg, & Ahlsén, 2009).
However, thier attitudes about AAC intervention range from acceptance to rejection or abandonment of AAC systems (Baxter, Enderby, Evans, & Judge, 2012; Johnson, Inglebret, Jones, & Ray, 2006; Moorcroft, Scarinci, & Meyer, 2019; Park, 2020; Park, Lee, & Park, 2020). Parents who accepted AAC treatment approaches for their children are more committed to interventions (Golbart & Marshall, 2004; McNaughton et al., 2008; Parette Jr, Brotherson, & Huer, 2000). These parents take an active role in determining the AAC device options and setting up the intervention goals, and they actively participate in promoting their children’s AAC use in their daily lives (Marshall & Goldbart, 2008). Conversely, parents with a negative attitude and an incomplete knowledge are apt to believe in misconceptions about AAC, and often prefer to rely only on traditional treatment approaches to improve their children’s speech production. Past experiences with less than successful AAC interventions can also influence parents’ attitudes (Moorcroft et al., 2019). Some common misconceptions described by Romski and Sevcik (2005) include: that AAC may hinder children’s speech development; that it should only be considered when other treatments have proven ineffective; and that only children with normal cognitive abilities can use speech-generating AAC devices. Such misconceptions increase the chance of missing the critical point for providing appropriate interventions for the child (Cress & Marvin, 2003).
According to previous studies conducted in Korea, parents of children with disabilities generally lacked understanding and information about AAC, and therefore needed specialized education and service programs to utilize AAC. For example, Lim, Park and Ku (2013) conducted individual and focus group interviews with 10 parents of children with developmental disabilities. The reasons for the difficulty in accepting AAC were the lack of information and data on AAC, the negative perception of special education teachers, and lack of professionalism, etc. Oh (2018) also found that there was a lack of information and negative perceptions about AAC through in-depth interviews with mothers of children with disabilities who are not using AAC. In addition, Shin and Lee (2016) confirmed that parents of students with disabilities had low awareness and support for AAC. They argued that parent education, expert training, and the strengthening of public relations were necessary to raise awareness. In particular, several studies showed that there was a high demand for AAC device-related information and education (Angelo, Jones, & Kokoska, 1995; Bailey, Parette Jr, Stoner, Angell, & Carroll, 2006; McNaughton et al., 2008; Park et al., 2020).
In this regard, the role of speech-language pathologists (SLPs) in providing AAC training and information for parents and families is emphasized (Baxter et al., 2012; Moorcroft et al., 2019). This is not only needed while AAC assessment and intervention services are being provided to the child, but also prior to providing services to correct any misconceptions the parents may have. The importance of SLPs’ role in educating parents is particularly emphasized in countries including Korea in which awareness of AAC has not yet been established due to insufficient and inaccurate information provided to them. Thus, giving parents the opportunity to obtain information regarding AAC (e.g., definition, purpose, candidates, types of AAC systems, AAC use strategies, policies and funding etc.) through online or offline seminars or individual education program can be helpful to them. In particular, parents who lack opportunities to become familiar with AAC devices have a particular need to be educated on how AAC communication works. Having them experience AAC devices can help them integrate their family values, routines, and preferences into the decision-making process of selecting the most appropriate AAC device and options for their children. In this way, they may gain a sense of ownership and the motivation to make full use of AAC systems (Jones, Angelo, & Kokoska, 1999; Moorcroft et al., 2019; Parette Jr et al., 2000).
To provide evidence about the effect of parent education on AAC perception, this study developed the parent education program which focused on correcting misconceptions about AAC, providing relevant information, and having device trials. The specific research aims are, (1) to determine whether there is a significant difference in the AAC perception scores between pre- and post-education, and (2) to examine whether there is a significant relationship between satisfaction with the program and change in the AAC perception scores.
METHODS
Participants
Twenty-five Korean mothers of children with spoken language challenges participated in this study. After sending an official letter related to the research to disability-related institutions in Daejeon City, the primary researcher recruited participants through telephone and e-mail. The mean age of mothers was 39.12 years (SD=3.56, min=30, max=47) and the mean years of education was 15.20 years (SD=1.88, min=12, max=18). Among the participants, six were high school graduates, 17 were university graduates, and two were graduate school graduates. They were all residents of Daejeon in the Republic of Korea and spoke Korean as their mother tongue.
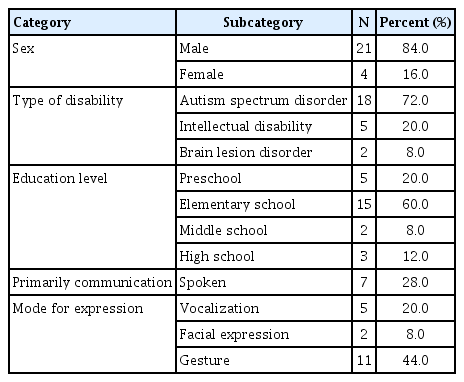
As shown in Table 1, the children of the participants consisted of 21 males and four females. The mean age of the children was 9.40 years old (SD=3.98, min=3, max=18). Five were in preschool, 15 in elementary school, two in middle school, and three in high school. The children had autism spectrum disorder (n=18, 72%), intellectual disability (n=5, 20%), and brain lesion disorder (n=2, 8%). The main communication mode for expression was gestures (n=11, 44%), followed by speaking (n=7, 28%), vocalization (n=5, 20%), and facial expressions (n=2, 8%). 16 participants (64% of the total) reported that the intelligibility of their children’s speech was too low for comprehension. Seven of 16 participants stated that they could not understand a single word of their children’s speech. The rest of the participants (n=9) reported that they had no difficulty or only slight difficulty understanding what their children said but that their expressive language skills and the number of words that they can express were limited. The seven children surveyed who communicated verbally were found to have very low speech intelligibility for comprehension, or a very limited number of single-word utterances. Regarding children’s receptive language skills, two children did not understand at all, nine children showed word level comprehension, and 14 simple phrase/sentence level comprehension. The mean years of the speech-language therapy that the children received was 6.22 years (SD=3.13, min=1.5, max=14).
Education Program and Material
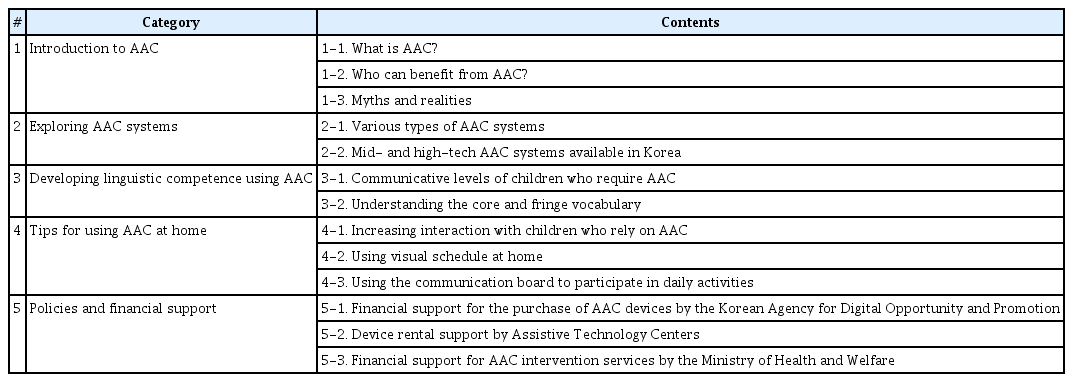
The education program was designed as one visit and was developed by reviewing published literature on AAC (e.g., Beukelman & Mirenda, 2013; Ganz, 2014; Light, Beukelman, & Reichle, 2003). In addition, policy and funding information was included to financially support the parents who would need the AAC services. As shown in Table 2, the program consisted of five sections: (1) Introduction to AAC, (2) Exploring AAC systems, (3) Developing linguistic competence using AAC, (4) Tips for using AAC at home, and (5) Policies and financial support. These sessions were conducted in numerical order. A booklet covering all the sections was developed (see Appendix 1). The booklet consisted of a total of 10 pages excluding the table of content and all sessions were equally composed of two pages. The education program and the booklet were reviewed by a professor who received their doctorate in the field of AAC.
Participants were provided with the opportunity to try several AAC systems to expand their awareness of AAC options for their children’s communication during the second section, that is exploring AAC systems. Two mid-tech devices available in Korea (Go Talk 20 plus [Attainment Company, n.d.]; OK Talk Talk (Version 1.0.5) [Geni Cube, 2016]) and two high-tech AAC applications (My Talkie Smart [Voiceware, 2018]; My AAC - for general use [NC Foundation, 2017]) were tried during the parent education. Following the researchers’ modeling, participants used the devices to select symbols and form simple sentences.
Development of Survey Questionnaires
First, to measure the effect of parent education on parents’ AAC perception, survey questionnaires consisting of 8 items were developed based on literature that discusses misconceptions about AAC (Bailey et al., 2006; Cress & Marvin, 2003; Romski & Sevcik, 2005; Smith, Barton-Hulsey, & Nwosu, 2016; Starble, Hutchins, Favro, Prelock, & Bitner, 2005). Surveys were conducted with the same questionnaires before and after providing parent education. Participants were asked to respond to each item regarding an AAC misconception using the 5-point Likert scale (1=strongly agree, 2=agree, 3=neutral, 4=disagree, and 5=strongly disagree).
Next, another set of survey questionnaires was developed to examine the relationship of participants’ change in perception of AAC with their satisfaction with the parent education, also on the 5-point Likert scale. It consisted of 8 items on a variety of aspects of the program (e.g., overall satisfaction with the education program, appropriateness of the amount of time it took, ease of understanding, and helpfulness with AAC devices).
The content validities for the two survey questionnaires were obtained by two raters who are professors in the Department of Speech & Language Pathology and have more than 10 years of education, research, and clinical experience in the AAC field.
Procedure
Given that in the clinical settings, clinicians often provide information about AAC to individual parents and answer questions related to their children, parent education was provided to each participant by a single researcher, mainly from the speech therapy center at the University. If necessary, the researcher visited the participant’s home or any private and quiet place such as a room at a special education school or a local facility for people with disabilities.
After obtaining signed consent forms from the participants, a pre-survey on parent perceptions was conducted before the parent education. Parent education was designed with 40 minutes of content. Including the question-and-answer time, sessions lasted for 1 to 1.5 hours. The length of sessions did not exceed 1.5 hours in consideration of the concentration and fatigue of the participants. After the parent education, each participant completed a post-survey on AAC perception followed by the survey on satisfaction with the program. The researcher left the room after verbally communicating to the participants the need for an objective evaluation, and the participants completed both surveys in the absence of the researcher.
The researcher who provided the education was a graduate student in speech-language pathology. The researcher spent six months developing the parent education program and preparing answers to potential questions related to the communication challenges and AAC approaches of the research participants. This preparation phase was completed so that the researcher could provide correct, reliable, and helpful information to parents, and this phase was reviewed and monitored by the professor whose primary research and clinical area is AAC.
Data Analysis
To determine whether there was a significant difference between the pre- and the post-surveys on AAC perception, a paired t-test was performed for each survey item. Also, a repeated measures ANCOVA was conducted on the total pre-survey scores and the total post-survey scores to examine whether other child-relevant variables such as age duration of speech therapy would impact on parents’ perceptions.
To identify any significant correlation between the satisfaction with the program and the change in AAC perception, a Spearman correlation coefficient analysis was performed. To run the analysis, the total satisfaction scores were computed by summing the 8 survey items’ scores for each participant. Change in AAC perception was computed by subtracting the total pre-survey scores from the total post-survey scores for each participant. IBM SPSS Statistics version 26 was used for statistical analyses.
RESULTS
Changes in AAC Perception Following the Provision of Parent Education
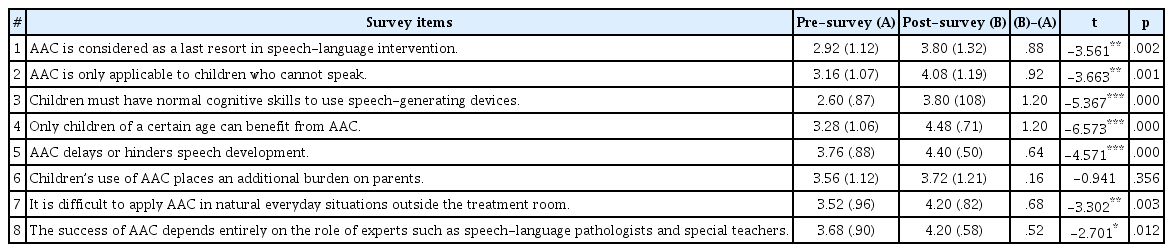
The mean AAC perception scores obtained by the sum of presurvey scores and the sum of post-survey scores for 25 participants divided by 25 were 26.48 (SD=4.08) and 32.68 (SD=4.27), respectively. The mean scores for all survey items increased at post-survey and the differences between pre- and post-survey scores were all significant except for the survey item “Children’s use of AAC places an additional burden on parents” (Table 3). The biggest change was observed in the survey items “Children must have normal cognitive skills to use speech-generating devices” (mean difference=1.20) and “Only children of a certain age can benefit from AAC” (1.20). The former item was the one which showed the lowest mean scores at the pre-survey. The item with the next highest difference was “AAC is only applicable for children who cannot speak” (.92), followed by “AAC is considered as a last resort in speech-language intervention” (.88) and “It is difficult to apply AAC in natural everyday situations outside the treatment room” (.68).
In addition, the repeated measured ANCOVA showed that the difference between the total scores of pre-and post-surveys was significant (F=17.164, p<.001). Age of children and duration of speech-language therapy had no effect on the perception change as covariates.
Correlation with Satisfaction of Parent Education Program
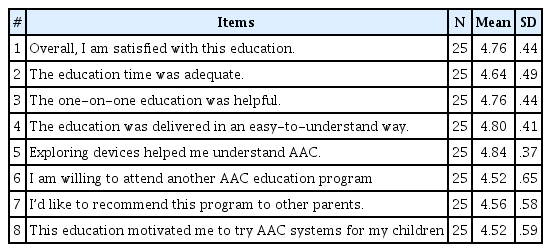
Participants showed relatively high satisfaction with the parent education (Table 4). The highest mean score was 4.84 (SD=.37) for the survey item “Exploring devices helped me understand AAC” followed by “The education was delivered in an easy-to-understand way” (M=4.80, SD=.41), “The one-on-one education was helpful” (M=4.76, SD=.44), “Overall, I am satisfied with this education” (M=4.76, SD=.44), “The education time was adequate” (M=4.64, SD=.49), “I’d like to recommend this program to other parents” (M=4.56, SD=.58), “I am willing to attend another AAC education program” (M=4.52, SD=.65), and “This education motivated me to try AAC systems for my children” (M=4.52, SD=.59).
The Spearman’s rho was .443 (p=.027), indicating a moderate positive correlation between the degree of satisfaction and the change in AAC perception.
DISCUSSION & CONCLUSION
The importance of parent education regarding AAC has been emphasized in previous studies (e.g., Anderson, 2015; Parette Jr et al., 2000; Thunberg et al., 2009) but without empirical evidence of its impact on AAC perception. This study showed that parent education focused on correcting misconceptions about AAC and providing relevant information had a positive effect on parents’ perceptions of AAC. These results are consistent with previous studies that AAC family support leads to changes in parents’ perceptions and attitudes (Kim & Park, 2003; Kim & Park, 2012) and that parent education is effective in raising awareness of the use of AAC (Bruno & Dribbon, 1998; Fanale, 2013). As studies have raised the need for family support and parent education (Anderson et al., 2015; Angelo et al., 1995; Lim et al., 2013; Park, 2020; Shin & Lee; 2016), and this study came to the conclusion that the parent education has a positive effect on improving their AAC awareness, it is necessary to develop a plan for the continuous development and spread of parent education programs.
Interestingly, the mothers who participated in this study were found to be somewhat at odds with the idea that AAC impedes their children’s speech development even before they were educated. This is quite different from the results of previous studies that AAC causes children to give up speech production and negatively affects speech therapy (Oh, 2018; Shin & Lee, 2016). This difference may be due to the demographic characteristics of the parents who participated in each study. Also, there is a possibility that the previous exposure to AAC education and/or training might affect the parents’ perception. Therefore, we cannot generalize this finding to parents in other cities or countries, as they may show different responses for each misconception depending on their existing levels of knowledge and experience with AAC.
Looking at the characteristics of the participants who had a relatively strongly negative perception of AAC, it was found that mothers had no prior information and experience with AAC, their children were older than middle school, or their children had more than 7 years of speech therapy experience. It seems that the burden and concern about a new communication system formed a negative perception of AAC (Goldbart & Marshall, 2004; Jones et al., 1999). It also shows that accurate information about AAC was not communicated to parents while receiving speech therapy for a long time. This demonstrates the importance of parent education.
The change of perception due to parent education highlights the role of SLPs in building parents’ motivation to participate in their child’s intervention phases (Baxter et al., 2012; Moorcroft et al., 2019). This study did not show explicitly whether Korean parents whose perception of AAC demonstrated improvement would actually adopt an AAC system to help their children communicate. However, the result of the satisfaction survey indirectly indicates a potential increased likelihood of adopting the AAC system. That is, mothers rated the survey item “This education motivated me to try AAC system for my children” highly (M=4.52, which is between “agree” and “strongly agree”).
Correlation of satisfaction with perception of AAC was found to be moderate. It seems that this is because the Korean parents gave high scores in general. Nevertheless, the significant correlation indicates that the parent education’s delivery of AAC information and the opportunity for familiarization with the devices is a welcome way for parents to raise their awareness. In cases where the parent lacks experience with AAC devices and this lack impacts their understanding of AAC, we recommend including a device trial session in the program. One-on-one education is also recommended if parents wish to receive more specific information related to their children. Previous studies have also discussed the effectiveness of one-to-one consultation and device experience opportunities (McNaughton et al., 2008; Parette Jr et al., 2000; Starble et al., 2005).
It should be noted that this study measured only the short-term effect of parent education on AAC perception without any comparison group. Further study will be needed to confirm whether changes in parents’ perceptions and attitudes can play a role in their engagement in AAC intervention phases, as opposed to parents who have not been educated as here described. Another limitation of this study is that, as already mentioned, the cultural characteristics of Korea may have influenced the study results. For example, the fact that the recruited participants were all mothers and that it is not easy for them to access information on AAC devices and policies in Korea in particular may lead to different results from studies done in other countries. Therefore, when conducting parent education, it is recommended to modify the contents and composition of the education used in this study according to the actual situation of the country and the target parents. Lastly, this study devised a parent education program that can be directly applied to the parents of children with various disabilities in the field. Therefore, the type of individual children’s disabilities and their ages were not controlled when recruiting the research participants. However, if an education program is developed according to the individual type of disability and age, it is expected to be of greater help to parents.