A normal swallow results in food, liquid, or other substances moving safely and efficiently from the mouth to the stomach. Proper deglutition or safe transport of food and liquid to the stomach is critical to survival and nutrition. A safe swallow is important not only for maintaining a healthy nutritional status, but also to improve one’s quality of life (Robbins, Hamilton, Lof, & Kempster, 1992).
A swallowing disorder, referred to as dysphagia, is any difficulty in the transfer of food or liquid from the mouth to the stomach (Groher, 1997). Dysphagia can negatively impact health, nutritional status, quality of life, and even result in death in poststroke patients (McHorney et al., 2000). It is essential to identify and treat dysphagia, as it can lead to dehydration, malnutrition, and aspiration pneu-monia, which over 40% of hospitalized elderly patients have (Langmore et al., 1998; Logemann, 1998).
Dysphagia resulting from a stroke affects the physiological swallowing response in the oral cavity, pharynx, and larynx (Logemann, 1995). Poststroke patients have difficulty of swallowing due to impaired motor and sensory functions in the oral and pharyngeal stages of swallowing (Groher, 1997). Between 30% and 50% of poststroke patients have swallowing problems (Kidd, Lawson, Nesbitt, & MacMahon, 1993; Mann, Hankey, & Cameron, 1999). Dysphagia after an acute stroke in elderly patients is more severe than age-related swallowing problems (Martino et al., 2005). Poststroke patients who aspirate are 7.5 times more likely to develop pneumonia when compared to those who do not (Schmidt, Holas, Halvorson, & Reding, 1994).
Videofluorographic Swallowing Examinations (VFSEs) are per-formed to examine the anatomy and physiology of oropharyngeal swallowing. VFSEs provide frame-by-frame video X-rays of oropharyngeal swallowing (Logemann, 1998). During VFSEs, various bolus consistencies can be examined. Barium is mixed with different consistencies from thin to solid consistency, and with different volumes from 1 to 10 mL.
Pharyngeal dysphagia can be categorized depending on where, how far, and whether or not the bolus enters the airway. Penetration occurs when the material being swallowed enters the airway but does not pass below the true vocal folds. Aspiration is when the material passes the true vocal folds and is not ejected from the trachea, possibly entering into the lungs (Robbins, Coyle, Rosenbek, Roecker, & Wood, 1999). Penetration-aspiration scale (P-A scale) can be used clinically to identify and quantify penetration and aspiration. The depth of airway invasion, cough reflex, and the ability to clear the airway of the penetrated or aspirated material were considered in the development of the P-A scale (Robbins et al., 1999). Research has found that the P-A scale is accurate in identifying penetration and aspiration with healthy elderly individuals and elderly poststroke patients. Scores range from one to eight; two to five indicate penetration, six to eight indicate aspiration with eight being silent aspiration.
In patients with dysphagia, higher aspiration rates in thin liquids were observed compared to thicker liquid consistencies (Kuhlemeier, Palmer, & Rosenberg, 2001). Therefore, thicken liquids are one of the most frequently used compensatory strategies in hospitals and long-term care facilities (Garcia, Chambers, Matta, & Clark, 2005; Robbins et al., 2002). Modifying bolus consistencies is believ-ed to promote safe swallowing and minimize the risk of aspiration (Garcia, Chambers, & Molander, 2005).
Changes in bolus consistencies have also been shown to influence the physiology of swallowing in normal and poststroke patients (Dantas et al., 1990). Thickened liquids, such as honey or nectar thick liquid consistencies, are used when patients exhibit poor oral control, delayed pharyngeal response, poor airway protection, or reduced sensory or cognitive awareness (Lazarus et al., 1993).
Previous studies have evaluated the effect of various bolus consistencies on temporal measurements, but only a few studies have examined the effects of bolus consistencies on swallowing safety in poststroke patients. In addition, it is important to determine whether there is difference within various consistencies on swallowing safety. Determining the effects of bolus consistencies on the safety of swallowing during the pharyngeal stage of swallowing can provide insight into which bolus consistencies result in safer swallows and corresponding diet recommendation for poststroke patients with dysphagia.
The purpose of this study was to determine whether different bolus consistencies (thin liquid, nectar thick liquid, and puree) would improve the safety of swallowing and whether there would be a difference within these consistencies on swallowing safety in poststroke patients with aspiration. The P-A scale was used to quantify whether the changes of bolus consistencies reduce the risk of penetration or aspiration in elderly poststroke patients. Examining the effects of three different bolus consistencies on the safety of swallowing in poststroke patients may provide information to implement effective swallowing management strategies for poststroke patients with dysphagia.
METHODS
Subjects
VFSEs of 24 poststroke patients from a previous investigation were analyzed for this study (McCullough, Wertz, & Rosenbek, 2001). Among them, twelve poststroke patients who had exhibited aspiration in thin liquid were then advanced to thick liquids and puree participated in the data analysis in this study. The mean age of the poststroke patients was 66.25 years. Days post onset of stroke ranged from one to 34. Table 1 provides the descriptive data with reference to the poststroke patients.
Videofluoroscopic Swallowing Examination Procedure
VFSEs were taken of the patients by having them seated upright in a stretcher chair for the duration of the examination. VFSEs were conducted with a mobile, C-arm X-ray system (model 7600; OEC Medical Systems, Salt Lake City, UT, USA). The studies were recorded with a Panasonic Super VHS PV-S7670 Pro Line Multiplex videocassette recorder. The fluoroscopic tube was focused on the oral cavity from the lips anteriorly to the pharyngeal wall posteriorly, and from the nasopharynx superiorly to just below the area of the upper esophageal sphincter (McCullough et al., 2001).
The clinicians instructed each patient to swallow after putting the liquid in his/her mouth by pill cup. Examinations were observ-ed from two 5-mL swallows of thin liquid with a viscosity 14 cP (centipoise). The mixture consisted of water and E-Z-HD barium sulfate powder for suspension. The patient then swallowed two 5-mL swallows of thick liquid with a viscosity of 187 cP. The thick liquid was a mixture of thickened juice and E-Z-HD barium sulfate powder for suspension. The final swallow observed was one 5-mL bolus of puree (applesauce) mixed with E-Z-HD barium sulfate powder for suspension from a spoon.
Procedure of Penetration-Aspiration Scale and Training
Five swallows of each patient were analyzed: two thin liquid, two nectar thick liquid, and one puree for a total measurement of 60 swallows. Each VFSE was first examined for anatomical structures and abnormalities and then the entire swallow was examined to evaluate the bolus flow. Each swallow was submitted to slow motion and frame-by-frame analysis using the Adobe Premier Pro ver. 1.5. The P-A scale was used to quantify each swallow with the following rating: one, normal; two to five, penetration; and seven to eight, aspiration. In addition to the score, the depth of the airway invasion, cough reflex, and the ability to clear the airway of penetrated or aspirated material were also noted (Robbins et al., 1999; Rosenbek, Robbins, Roecker, Coyle, & Woods, 1996).
Statistical Analysis
Statistical comparisons were made by using one-way analysis of variance (ANOVA). The independent variables were the three bolus consistencies. The dependent variable was the P-A scale measurement. Significance level was set at p<.05. A post-hoc test (Tu-key) was performed to determine the significant difference of the three bolus consistencies.
RESULTS
Reliability
Intra- and inter-judge reliabilities were established using interclass correlation coefficient (ICC). For intra-judge reliability, the principal investigator with two years of training at swallowing research randomly selected and re-analyzed 33% of the VFSE clips (4 subjects). A significant correlation between the first and the second set of recordings was observed, as r values obtained were greater than 0.80 (r=.86, p<.01). For inter-judge reliability, a second judge analyzed 33% of the VFSE clips (4 subjects). The second judge was a doctoral student with three years of training using the P-A scale on VFSE clips. The second judge’s results were compared to the primary investigator’s results, and a significant correlation was observed between the ratings as r values obtained were greater than 0.80 (r=.84, p<.01).
Poststroke Patients with Aspiration
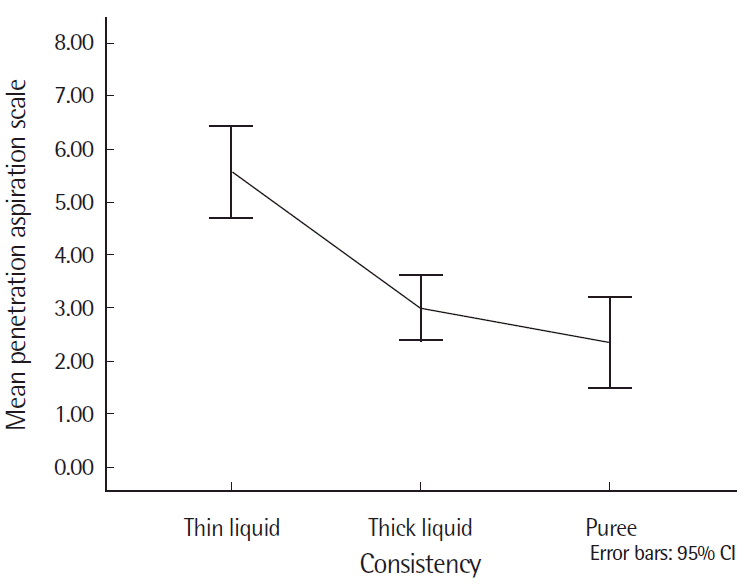
Table 2 provides the mean and SD for the three bolus consistencies among poststroke patients with aspiration. The mean P-A scale value decreased from the thin liquid to the puree. The poststroke patients with aspiration displayed mean P-A scale values of 5.75 (SD=1.91) for thin liquids, 3.08 (SD=1.44) for nectar thick liquids, and 2.41 (SD=1.24) for puree consistencies. Thin liquids had the highest P-A scale values for poststroke patients with aspiration when compared to nectar thick liquid and puree consistencies, suggesting that thickening the bolus can result in a safer swallow. Figure 1 displays the mean and 95% confidence interval for P-A scale values among the three bolus consistencies in poststroke patients with aspiration.
Table 3 provides post-hoc analysis of P-A scale values among the three bolus consistencies for poststroke patients with aspiration. Significant differences were observed between thin liquids and nectar thick liquids (p<.01) and between thin liquids and puree (p<.01). No significant difference was observed between nectar thick liquids and puree consistencies (p=.55).
CONCLUSION
This study aimed specifically to determine whether different bolus consistencies (thin liquid, nectar thick liquid, and puree) would improve the safety of swallowing and whether there would be a difference within these consistencies on swallowing safety in poststroke patients. Bolus consistencies were examined since modifying bolus consistencies is believed to promote the safety of swallowing and minimize the risk of aspiration (Garcia, Chambers, & Molander, 2005). In addition, thickened liquids or pureed foods are one of the most frequently used compensatory strategies for patients who aspirate thin liquids (Robbins et al., 2002). The safety of swallowing was measured using the P-A scale.
The results of this study for poststroke patients with aspiration indicated that changing the bolus consistency from thin liquid to nectar thick liquid and from thin liquid to puree reduced the P-A scale values significantly; however, no significant differences were found between nectar thick liquids and puree. The findings have two clinical implications. First, thickened liquid provided an alternative way to obtain liquid or food safely to poststroke patients who aspirated thin liquid. Second, in poststroke patients with aspiration, there is no difference in swallowing safety between nectar thick liquid and puree consistency.
The significant differences between thin liquid and nectar thick liquid and between thin liquid and puree for poststroke patients with aspiration may be due to the change in viscosity of the bolus. Thicker bolus consistencies move slowly in the oral and pharyngeal cavities, thus increasing bolus transit time, which allows the poststroke patients with aspiration to compensate for a delayed pharyngeal swallow and let them have more effort to swallow. This effort increases the distance of hyoid and laryngeal excursion and increases the duration of the upper esophageal sphincter opening during the pharyngeal swallow (Bisch, Logemann, Rademaker, Kahrilas, & Lazarus, 1994; Dantas et al., 1990; Lazarus et al., 1993). Therefore, thickened liquids which form a cohesive bolus are preferred in poststroke patients who have difficulty swallowing thin liquid (Garcia, Chambers, & Molander, 2005).
Based on the results of this study, both thickened liquids and pureed food can be used to reduce the risk of aspiration in poststroke patients with aspiration. Patients, caregivers, and clinicians may have a variety of options for diet medication. Clinicians and patients are able to perform intervention exercises with modified bolus. However, since diet modification like thickened liquids or pureed food can only be a short-term compensation strategy, it is important to develop an intervention plan to fit nutritional and psychosocial needs in terms of quality of life in poststroke patients. Other factors, such as oral strength and hygiene, cognition and motivation to participate in rehabilitation exercises, should be considered as well.
VFSEs allow clinicians to observe bolus flow, residue, and the presence of penetration or aspiration during the oropharyngeal swallow. The subjects of this study showed aspiration with thin liquid which is a greater risk for aspiration when compared to thicker consistencies (Kuhlemeier et al., 2001). When viewing VFSEs, the P-A scale is a useful tool for assessing swallowing and determining a safe consistency for poststroke patients. The P-A scale provides quantitative information regarding the safety of swallowing and can be used to monitor the progress of the treatment for patients.
This study had several limitations. The poststroke patients in this study were a heterogeneous group in terms of the site of lesion. Further, the study analyzed only three bolus consistencies—thin liquid, nectar thick liquid, and puree. All of the bolus volumes were 5 mL, not taking into consideration different bolus volumes. Future research should not only investigate additional bolus consistencies and volumes, but also consider the use of the P-A scale in conjunction with objective or quantitative measurements, such as biomechanical or temporal analyses of swallowing.
This study examined the effect of three bolus consistencies—thin liquid, nectar thick liquid, and puree—on the safety of a swallow for poststroke patients with aspiration. The P-A scale was used to measure the swallows quantitatively. A score of one to eight was given to each of the 5 swallows for the 12 subjects. While significant differences between thin liquids and nectar thick liquids and between thin liquids and puree were observed for the poststroke patients with aspiration, no significant difference was observed between nectar thick liquids and puree. This study suggests the following: for poststroke patients with aspiration, thin liquids have the highest risk for aspiration; thickening the liquids can improve the safety of a swallow; there was also no difference between nectar thick liquid and puree on swallowing safety. This study also validated that the P-A scale is a useful clinical tool for determining a safe consistency for poststroke patients and provides quantitative information regarding the safety of swallowing.